The Xclaims! Integrated Platform: Complete Revenue Cycle Control
The Xclaims! platform maximizes practice financial performance by reducing administrative burdens. Moving beyond basic clearinghouse functions, Xclaims! provides a suite of high-precision tools that allow billing staff to manage the entire revenue cycle from a single, centralized command center.
Claims Management
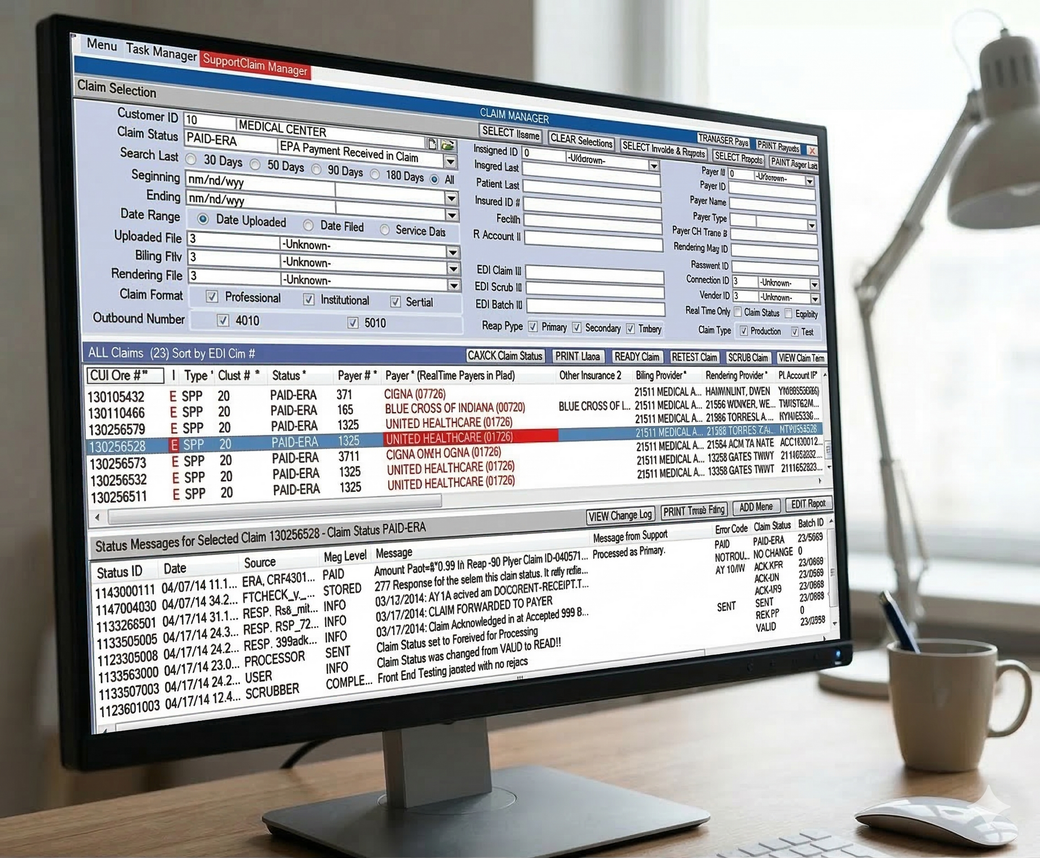
Xclaims! Claim Manager:
Accelerate Reimbursement and Maximize Revenue with Effortless Claims Control
Claim Manager is the core module and command center. It improves the billing and collections process from claim submission to workflow management. By streamlining operations, it enables faster reimbursements and greater revenue predictability. All claim activities are consolidated into a single platform, giving organizations a competitive edge by replacing fragmented, legacy workflows that increase the risk of missed deadlines, lost revenue, and heavier administrative workloads.
Claim Manager loads claims, automatically finds errors using our Clinical Claim Scrubber, and categorizes them as valid or invalid, enabling staff to focus corrections only where needed. Users manage the revenue cycle for each claim, including secondary and Workers’ Compensation claims.
98.5%
First-pass clean claim rate
Manage your entire claim lifecycle from a single screen.
Track real-time claim status and payer responses instantly.
Generate definitive proof of submission with a single click.
Core Capabilities
-
98.5% First-Pass Clean Claim RateItem Link List Item 2
Securely transmit claims to payers via a direct electronic interface.
High-precision scrubbing ensures the vast majority of claims are accepted on the first submission.
-
Real-Time Status TrackingItem Link List Item 3
Gain instant access to the current status and complete history of every claim, including all payer responses
-
Single-Screen WorkflowItem Link List Item 4
Review data, spot errors, and resubmit corrected claims from one simple screen. No more navigating between screens.
Picture this: it's a typical morning. Maria, your billing specialist, sees a claim flagged for an NPI mismatch. With everything on one screen, she quickly reviews, corrects, and resubmits the claim—without toggling windows. This workflow gives users total control, enabling them to resolve edits faster and with more confidence.
Integrated Timely Filing Protection:
Protect revenue by generating a 'Timely Filing Letter' with one click. This serves as financial insurance against revenue loss. It helps you challenge payer denials and prove on-time submission. By lowering the risk from missed deadlines, you reduce lost reimbursement and ensure consistent cash flow.
Secondary Claim Management
Automatically identify, create, and edit electronic secondary claims to capture all available reimbursement.
Workers' Compensation Support
Electronically file complex Workers' Compensation claims with the ability to submit all necessary supporting documentation.
Seamless PMS Integration
Connects directly with your existing Practice Management System to synchronize data and reduce manual entry.
Xclaims! Task Manager:
Master Your Workflow with Real-Time Actionable Intelligence
Eliminate Revenue Roadblocks with Automated Workflow Prioritization. Task Manager changes your billing department from reacting to problems to staying ahead of them by consolidating all important tasks into a single, easy-to-use dashboard. Instead of making staff search for mistakes in different reports, the system automatically identifies and routes rejected claims, denied ERAs, and invalid eligibility requests to the forefront of your workflow. This way, the most important tasks get handled first, preventing slowdowns and making sure every billable task is taken care of.
100%
Visibility of rejected claims and denied ERAs in a single view.
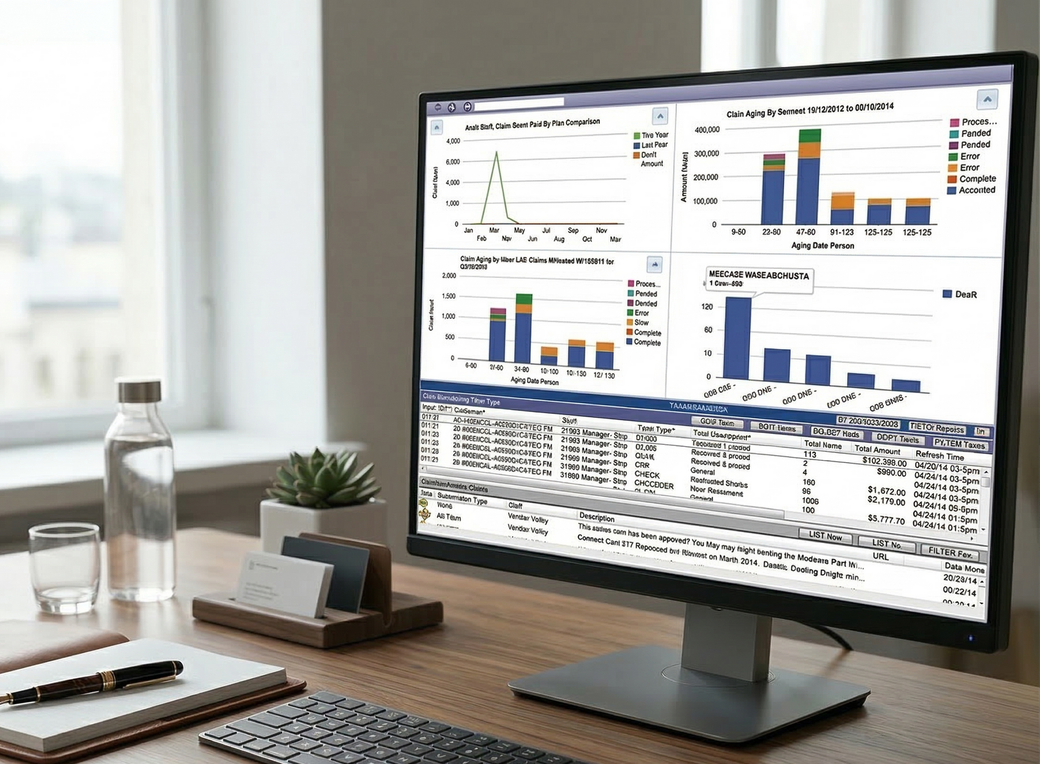
Automate tracking for every rejection to ensure no claim is left unpaid.
Replace manual task lists with a dynamic dashboard to organize daily work.
Monitor staff productivity and transaction aging across your entire organization in real-time.
Core Features
-
Multi-Module TrackingItem Link List Item 2
This integration allows users to create and manage tasks across all Xclaims! modules, including Claim Manager, Eligibility, and Support.
Our standard, full-functional integration means all task types are directly linked to their corresponding windows in Xclaims!. Users navigate and resolve issues without leaving the Task Manager screen.
-
Consolidated Support ManagementItem Link List Item 3
Track and manage open support issues alongside billing tasks within the same interface.
System totals are refreshed automatically as transactions are processed, providing real-time views of office productivity.
-
Customizable Selection CriteriaItem Link List Item 4
Build specific views by provider, aging, or dollar amount to match your practice's specific business needs, even down to diagnosis, CPT, or modifier codes within claims.
Tasks can be copied to multiple users or each user can have their own tasks built to suit their responsibilities.
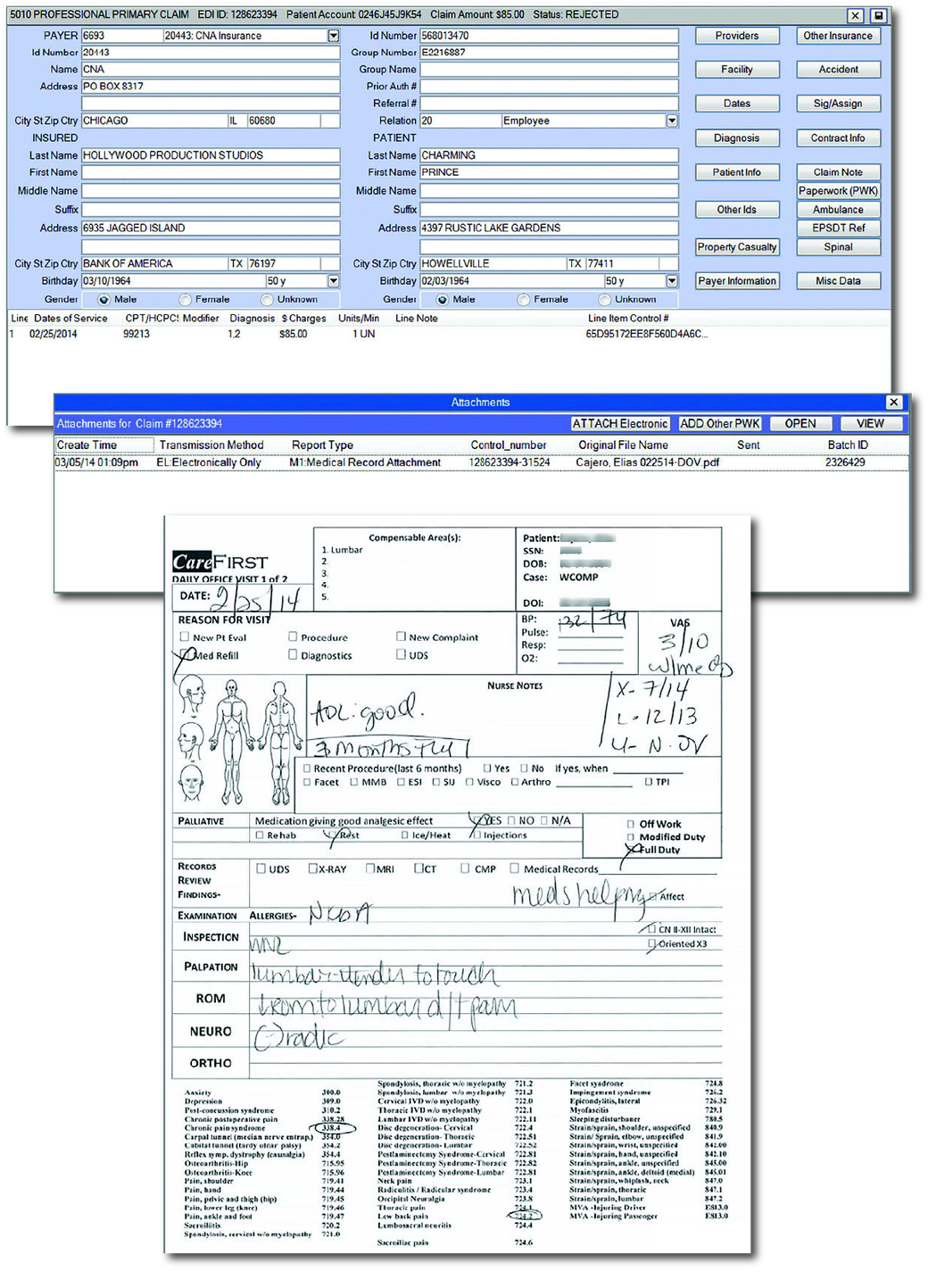

Workers’ Comp claims are often a major administrative burden due to the high volume of required supporting documentation. The Xclaims! The Workers’ Comp solution eliminates this manual labor by providing a fully electronic submission and management process. Through integrating documentation attachments directly into your workflow, Xclaims! assures that even the most complex injury claims are processed at the same speed and with the same transparency as standard professional claims.
Xclaims! Workers’ Comp & Auto Claims:
Accelerate Complex Submissions with 100% Electronic Workflow
100%
Workers' comp claim and documentation that is electronic
Eliminate the manual printing and mailing of case notes or lab reports by attaching unlimited digital documentation directly to any claim.
Stop managing Workers’ Comp as an outlier; track and manage these submissions electronically within the same interface as your other claims.
Simplify your workflow with an ergonomically integrated "Include Attachment" feature that reduces time per submission.
Core Features
-
100% Electronic SubmittalItem Link List Item 2
Submit both the initial claim and all required medical documentation to payers through a fully digital interface.
The system is designed for ease of use, making the addition of supporting files effortless during claim creation.
-
Unlimited AttachmentsItem Link List Item 3
Attach as many injury reports, case notes, or diagnostic results as necessary to satisfy payer requirements.
-
Management WorkflowItem Link List Item 4
Leverage the power of Xclaims! to monitor the status of Workers’ Comp claims alongside your standard revenue cycle.
Easily attach requested documentation to follow-up claims to resolve payer inquiries faster.
Payment Management
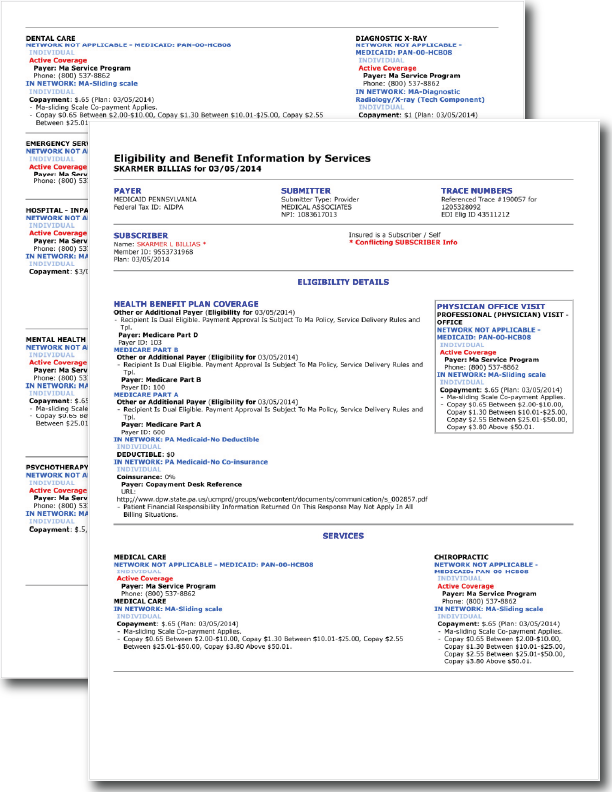

Stop losing the equivalent of hundreds of annual hours and thousands of payroll dollars to the "Free" Portal Myth. If your practice relies on phone calls and payer web portals to save money, the hidden labor costs are draining your bottom line. For example, in a 5-provider practice averaging 80 patient visits per provider per week, switching from manual portal checks to Imspro’s fully electronic workflow would recover over 5,300 staff hours per year—translating to more than $106,000 in annual labor savings at a typical $20/hour staff wage. Your staff recovers an average of 16 minutes per patient encounter.
As patient financial responsibility increases, the ability to secure insurance coverage in advance is essential for collecting payments onsite and maintaining cash flow. Xclaims! eliminates the traditional administrative burden of long payer hold times and the need to access multiple payor websites with immediate eligibility requests and responses within seconds on one platform.
Xclaims! Eligibility Verification:
Real-Time Benefit Clarity - Minus the Wait
16
Minutes saved per transaction compared to web portal verification
Stop the phone calls and website searches. Eligibility requests are processed instantly on a single platform, providing real-time access to coverage information.
Know exactly what to collect from patients before their visit or determine if they need to sign an ABN during their appointment.
Instantly identify, correct, and resubmit any eligibility requests returned as "Invalid" or "Rejected".
Core Features
-
Comprehensive DetailItem Link List Item 2
Reports show subscriber info, deductible status, co-insurance, co-payments, and specialty-specific benefit information.
Features a game-changing, consistently formatted report that is easy for staff to read and interpret.
-
Powerful Search/Filter/PrintItem Link List Item 3
Locate specific requests and responses by date, status, patient name, or payer.
Empowers front-desk staff with a comprehensive report of upcoming patients and their specific collection requirements.
-
One-Stop ProcessingItem Link List Item 4
Stop the phone calls and website searches. Eligibility requests are processed instantly on a single platform, providing real-time access to coverage information.
Easily submit one-off requests for unexpected or walk-in patients to ensure coverage is verified immediately.
The ERA Denial Manager changes how your practice deals with unpaid claims by turning payment data into an action plan. Instead of spending hours sorting through payment reports, this tool automatically flags every denial and sends it to the right staff member for immediate action. It also gives you real-time reports on your main denial reasons and which payers cause the most problems, so you can fix bigger billing issues and speed up your payments.
Xclaims! ERA Denial Manager:
Transform Denials into Useful Data
"Instantly"
Conversion of raw ERA data into actionable staff tasks.
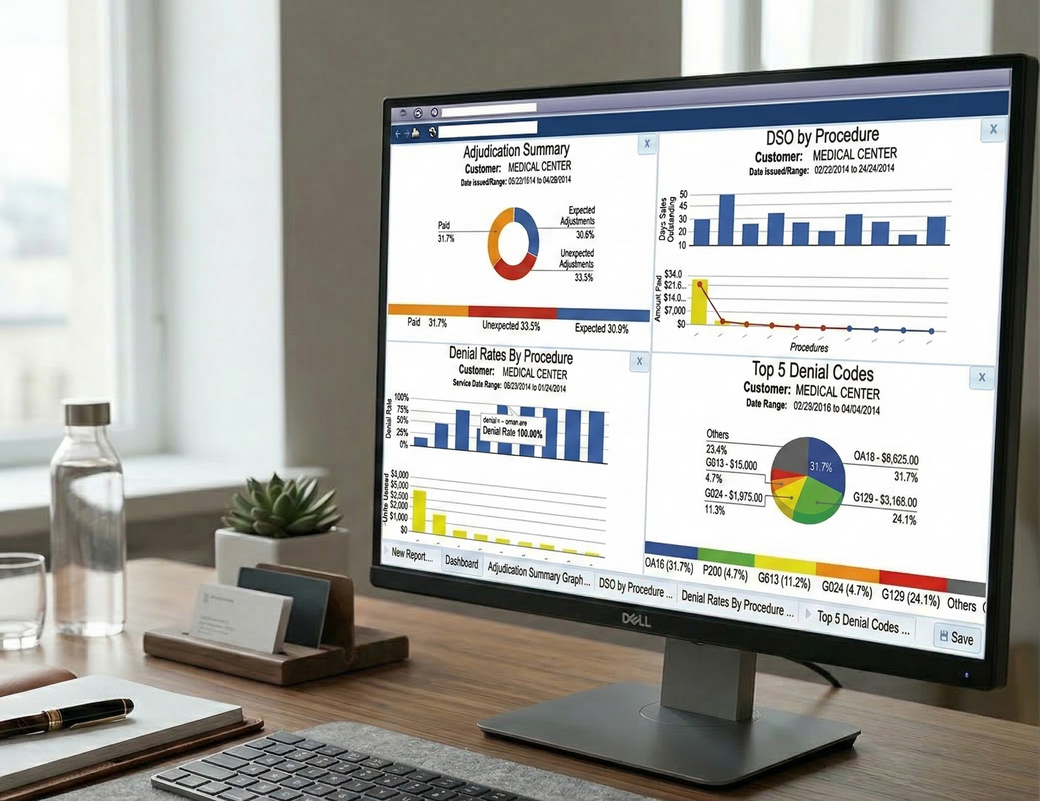
Identify exactly why claims are being denied (causing revenue leaks) with automated categorization and trend reporting.
Assign specific denied transactions to staff members and track their progress through to resolution.
Stop manually reviewing ERAs; use a dashboard to filter and prioritize denials by payer, reason, or dollar amount.
Core Features
-
Search & Filter Live DataItem Link List Item 2
Review ERA data as soon as it is received from the payer to reduce the time between a denied claim and its resubmission.
Quickly find transactions using multiple criteria, including patient name, check number, denial code, and more.
-
Statistical Trend AnalysisItem Link List Item 3
See full reports showing your most common denial reasons and which payers affect you the most.
See the exact codes and notes payers give for every part of a claim.
-
Integrated Task AssignmentItem Link List Item 4
Connect denied claims straight to the Task Manager, making sure every unpaid claim goes to the right team for follow-up.
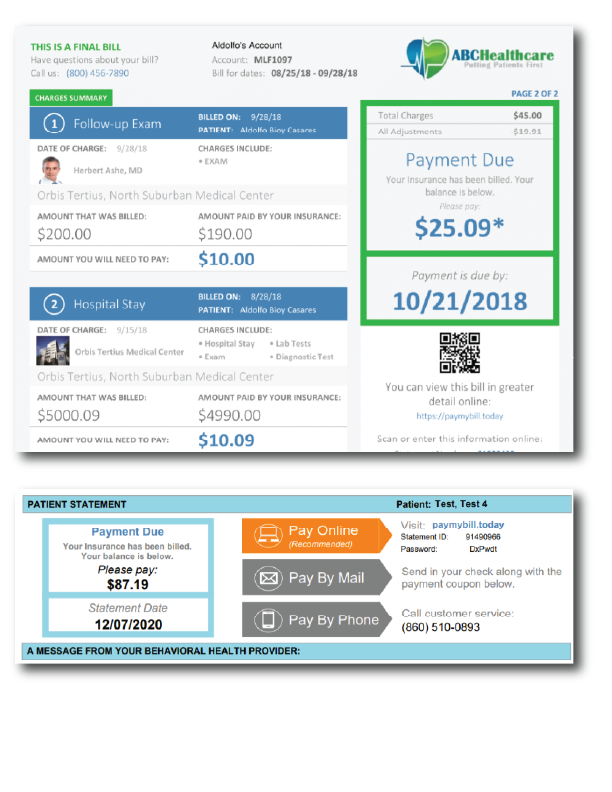
Guaranteed 24-Hour Processing to Turn Patient Balances into Practice Revenue.
Eliminate manual mailing processes that delay cash flow. Imspro’s integrated statement solution uses advanced processing technology to reduce administrative burden. Files transmitted to our secure portal by 4:00 PM CT are processed and mailed within one business day. The platform supports both paper mail and digital notifications, enabling faster delivery and reducing labor and supply costs.
Patient Statement & Letter Management:
Modernize Collections with High-Speed Delivery
24 Hours
Guaranteed processing and mailing for all statement files received by 4:00 PM CT.
24-hour processing ensures statements reach patients without delay while eliminating hours wasted on printing, folding, stuffing, and sealing envelopes.
Reach patients where they are, on their phones, with SMS and e-statement options that lead directly to payment.
Never navigate technical issues alone; your dedicated account manager is available via direct phone and email to support your process from transmission to delivery.
Core Features
-
Secure 24/7 PortalItem Link List Item 2
Transmit your files whenever your billing cycle is ready via our secure, encrypted portal, available 365 days a year.
Every file received by 4:00 PM CT is processed and delivered to the USPS within one business day.
-
Send & Pay OptionsItem Link List Item 3
Combine professional laser-printed paper statements with modern e-statements and SMS text notifications to fit patient preferences and save on postage.
Simplify the patient experience with mobile-friendly links that allow for instant balance settlement via text.
-
Advanced Postal AutomationItem Link List Item 4
Utilize Intelligent Mail Barcode (IMB) technology and presorting for the fastest possible delivery at the lowest postal rates.
Every account includes a US-based dedicated account manager with a guaranteed 2-hour response time for any processing questions.
Denial Prevention + Recovery

Denied and rejected claims are among the most costly, yet preventable, challenges a physician practice faces. The Xclaims! Clinical Claim Scrubber, powered by Aptarro, checks your claims for accuracy prior to submission by applying a pre-configured set of edits. Performing a standard structural validation alongside advanced clinical scrubbing, the system quickly returns clear, concise error messages in an integrated, easy-to-read response report, allowing your billing team to significantly clean up coding, reduce denials, and attain more accurate, optimal reimbursement.
Xclaims! Clinical Claim Scrubber:
Stop Denials and Rejections Before They Start
98.5%
Successful First-Pass Submissions
Identify medical necessity issues by checking CPT/ICD-10 combinations before the claim is sent.
Analyze claims from the payer's perspective to resolve possible issues and reduce overall AR days.
Stop searching through long reports; scrubber messages are parsed and attached directly to each invalid claim for immediate reference.
Core Features
-
Customizable EditsItem Link List Item 2
Create and configure edits customized to your practice's needs or specific payer and claim types.
-
Efficient WorkflowsItem Link List Item 3
Assign invalid claims to specific users based on error type to improve the correction process.
-
Intelligent Reporting:Item Link
Receive incredibly intuitive HTML response reports that can also be ported to your PMS via XML.
Comprehensive Review
Scrub both institutional and professional claims for structural and clinical accuracy.
Reimbursement Optimization
Sequence codes by the highest Relative Value Units (RVUs) to ensure you are maximizing your return.
Full ICD-10 Support
Complete support for all current ICD-10 procedure and diagnosis codes.
Custom Solutions for Your Practice

No two healthcare organizations operate the same way—so your clearinghouse shouldn’t either. Our platform is designed with flexibility at its core, adapting seamlessly to the unique requirements of multiple specialties, payer rules, and internal workflows.
We go beyond standard claim processing by offering custom-built edits and intelligent automation that help prevent denials before they happen. From specialty-specific billing nuances to payer-driven requirements, we tailor our solutions to fit your exact needs.
Our advanced workflow capabilities allow you to automate complex and exception-based scenarios, including:
- Holding claims until payer credentialing is complete
- Managing pre-payment review processes
- Supporting atypical provider billing scenarios without an NPI
We also develop targeted claim edits to ensure accuracy in even the most specialized cases—such as properly splitting claims for Rural Health Clinics (RHCs) and other unique billing structures.
The result? Fewer denials, streamlined operations, and a clearinghouse that works the way you do—not the other way around.
Imspro Custom Solutions
Flexible. Intelligent. Built Around You.
> 2,000
Custom Edits Currently In Use
"The absolute BEST Company"
Vickie Frith
Revenue Cycle Management Director
MRI Associates
View the entire testimonial, plus more, to see why our customers place their trust in Imspro.



